 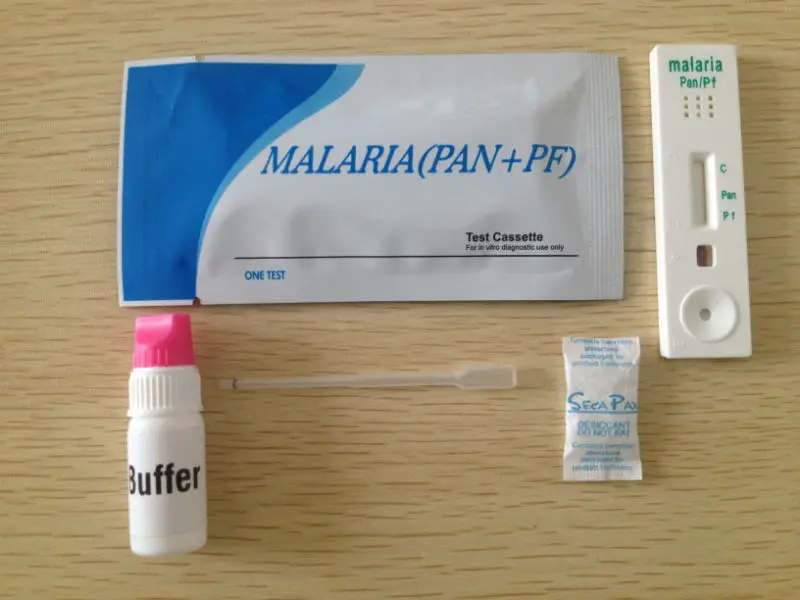 
Specifically, these tests can detect severe anemia, hypoglycemia, renal failure, hyperbilirubinemia, and acid-base disturbances. In the event that the person does have a positive malaria test, these additional tests will be useful in determining whether the patient has uncomplicated or severe manifestations of the malaria infection. Methods In this study, we collate all published and available unpublished. The test has already been used in many research studies in a wide range of geographies and use cases. In addition to ordering the malaria specific diagnostic tests described below, the health-care provider should conduct an initial workup and request a complete blood count and a routine chemistry panel. Background A new more highly sensitive rapid diagnostic test (HS-RDT) for Plasmodium falciparum malaria (Alere/Abbott Malaria Ag P.f RDT 05FK140, now called NxTek Eliminate Malaria Ag Pf) was launched in 2017. In severe malaria (primarily caused by Plasmodium falciparum), clinical findings (confusion, coma, neurologic focal signs, severe anemia, respiratory difficulties) are more striking and may increase the index of suspicion for malaria.Ĭlinical findings should always be confirmed by a laboratory test for malaria. Likewise, the physical findings are often not specific (elevated temperature, perspiration, tiredness). The first symptoms of malaria (most often fever, chills, sweats, headaches, muscle pains, nausea and vomiting) are often not specific and are also found in other diseases (such as the “flu” and common viral infections). The RDTs that can be procured through the Global Fund to Fight AIDS, Tuberculosis and Malaria are listed on the World Health Organisation's list of prequalified in vitro diagnostics.Clinical diagnosis is based on the patient’s symptoms and on physical findings at examination. vivax in samples containing 200 parasites/µL. Qualitative rapid diagnostic tests (RDTs), instead, do not require extensive sample preparation, provide detection limits comparable to microscopic thick smear analysis, and provide highly. As a consequence, many RDTs might fail to detect P. vivax infections, lower expression of the specific antigen being detected for this species, and poorer performance of the reagents used for this specific antigen. 3 This is due to a combination of lower parasite density in P. falciparum, and uptake has been slow and inconsistent. vivax have relatively poor performance compared with those for P. 
Guided by the Strategic Plan for 2022-2025 that aims to ensure that every child survives and. Malaria rapid diagnostic tests are the recommended form of confirmatory malaria diagnosis where microscopy is not feasible, for example, and especially, hard to reach areas. vivax clinical cases.Īntibodies and antigens currently used for the detection of Plasmodium spp. testing, either microscopy or a malaria rapid diagnostic test. vivax RDTs that do have significantly improved sensitivity – with the objective of reducing the number of missed P. falciparum, a number of initiatives are ongoing to develop P. 1 While the sensitivity of pLDH-detecting RDTs is often not as good as that achieved by HRP2-based RDTs for P. vivax is the parasite lactate dehydrogenase (pLDH). There the most suitable antigen for the species-specific detection of P. RDTs work by capturing dye-labelled antibodies bound to specific parasite antigens. They require no infrastructure or apparatus and can be used at the point-of-care, including in very remote areas. Regardless of the format, they are typically very simply to use, requiring no specialist services and minimal training. RTDs are available in various formats (dipstick, cassette or hybrids). These tests require a drop of peripheral blood, normally collected from a finger or heel prick. Visual read-outs are available typically within 20 mins or less. The accepted laboratory practice for the diagnosis of malaria is the preparation and microscopic examination of blood films stained with Giemsa, Wrights, or. Malaria rapid diagnostic tests (RDTs) assist in the diagnosis of malaria by detecting evidence of malaria parasites (antigens) in human blood.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
